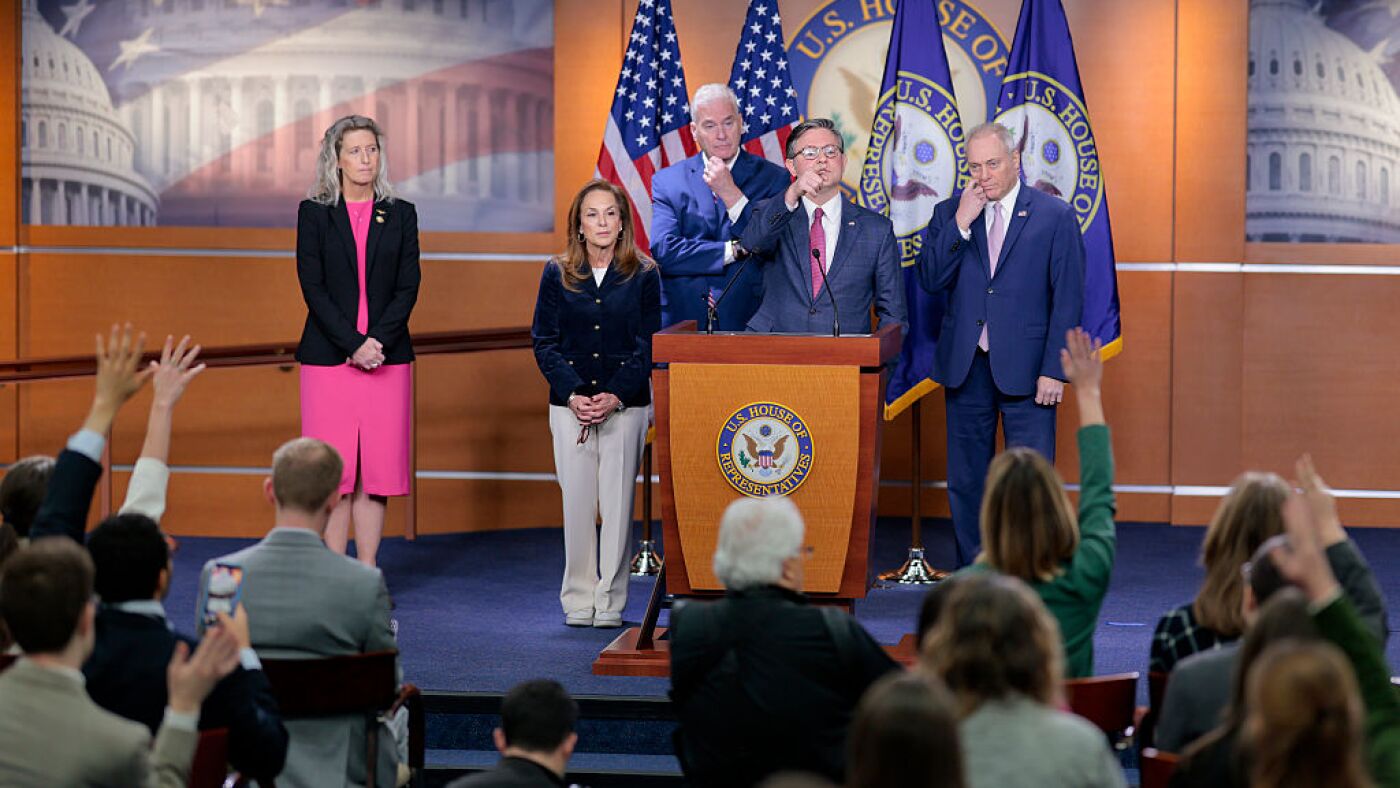Congressional Debate Puts ACA Subsidies in the Spotlight During Open Enrollment
As the debate over the future of the Affordable Care Act (ACA) intensifies in Congress, consumers are left grappling with uncertainty during this crucial open enrollment period. The discussions center around whether to extend subsidies that have helped many afford their health insurance premiums in recent years, adding a layer of complexity to an already challenging landscape.

Speaker of the House Mike Johnson, R-La., and other Republican leaders discussed health care plans with a vote regarding an extension of the ACA subsidies looming. Heather Diehl/Getty Images
A recent KFF poll highlights the potential political impact, with approximately half of ACA enrollees indicating that a $1,000 increase in healthcare costs could significantly influence their voting decisions in the upcoming midterm elections.
For the 20 states and the District of Columbia that operate their own ACA marketplaces, the lack of a resolution on Capitol Hill leads to uncertain planning for the year ahead. “Before I sign up, I will wait and see what happens,” commented Daniela Perez, a Chicago resident facing a significant jump in her insurance premiums without the extension of tax credits.
In recent Senate proceedings, a proposal to extend the subsidies failed to achieve the necessary votes. Meanwhile, the House, under Speaker Mike Johnson, is preparing a legislative package aimed at addressing healthcare costs by expanding association health plans and increasing transparency for pharmacy benefit managers.
While Democrats push to maintain the enhanced subsidies, created during the COVID-19 pandemic, Republicans are divided, with some concerned about the financial and political repercussions of extending support for a law they have long opposed. Nonetheless, some GOP members express concern about potential electoral consequences if subsidies are not extended.
Impact on Enrollment Numbers
Preliminary data from the Centers for Medicare & Medicaid Services shows a reduction in new ACA enrollments compared to the previous year, though returning customers have been quicker to select plans. This trend may indicate a heightened urgency among those with chronic health needs.
State-specific reports also indicate shifts, with Pennsylvania experiencing a 16% drop in new sign-ups, and California noting a 33% decrease. Affordability remains a critical issue, with many consumers opting for “bronze” plans, which offer lower premiums but higher deductibles.
Income levels play a significant role, as most cancellations in Pennsylvania came from individuals earning between 150% and 200% of the federal poverty level. The enhanced subsidies had allowed lower-income individuals to pay minimal or no premiums, a point of contention among Republicans.
Looking Ahead
As Congress deliberates, the deadlines for ACA enrollment loom, requiring marketplaces to prepare for potential changes. Audrey Morse Gasteier from the Massachusetts Health Connector stresses the importance of having a plan ready to inform consumers of any developments.
Jessica Altman from Covered California remarks on the ongoing challenges, noting, “In many ways, it feels like they are farther apart than they were even a few months ago.”
With fewer days left in the congressional calendar, the future of ACA subsidies remains uncertain, leaving Americans to watch closely as decisions unfold.